Neonatology: A Comprehensive Guide to Premature Baby Care and Treatment

Neonatology: Premature Baby Care and Treatment
A normal pregnancy typically lasts about 40 weeks. However, sometimes nature moves faster than expected, and a baby arrives before the 37th week.
This is where the most delicate and miracle-filled branch of medicine, neonatology, comes into play. Neonatology is a specialized science dedicated to protecting the health of newborns—especially those who open their eyes to the world early—supporting their development, and overcoming the medical challenges they face.
Preterm Birth and Neonatology
Preterm birth is not just about a baby being born early; it also means that their organ systems are not yet fully ready for the outside world.
In this process, the neonatology unit provides the necessary artificial environment and medical support for the baby to complete the development they would have had in the mother’s womb.
Neonatology specialists use all the possibilities of modern technology to monitor every breath of these tiny warriors and offer them the healthiest possible start.
Neonatologist: Who Are They and What Do They Treat?
A neonatologist is a medical doctor who has received advanced specialist training in the field of neonatology on top of their residency in pediatrics.
While neonatology specialists are responsible for all infants in the "newborn" period (the first 28 days after birth), their primary focus is on high-risk births.
Conditions treated by neonatology specialists include:
- Preterm birth (prematurity) and related complications.
- Situations involving a lack of oxygen at birth (Asphyxia).
- Newborn infections and sepsis.
- Congenital anomalies (birth defects).
- Pre- and post-operative care for newborn diseases requiring surgical intervention.
The Premature Baby: Definition and Classification
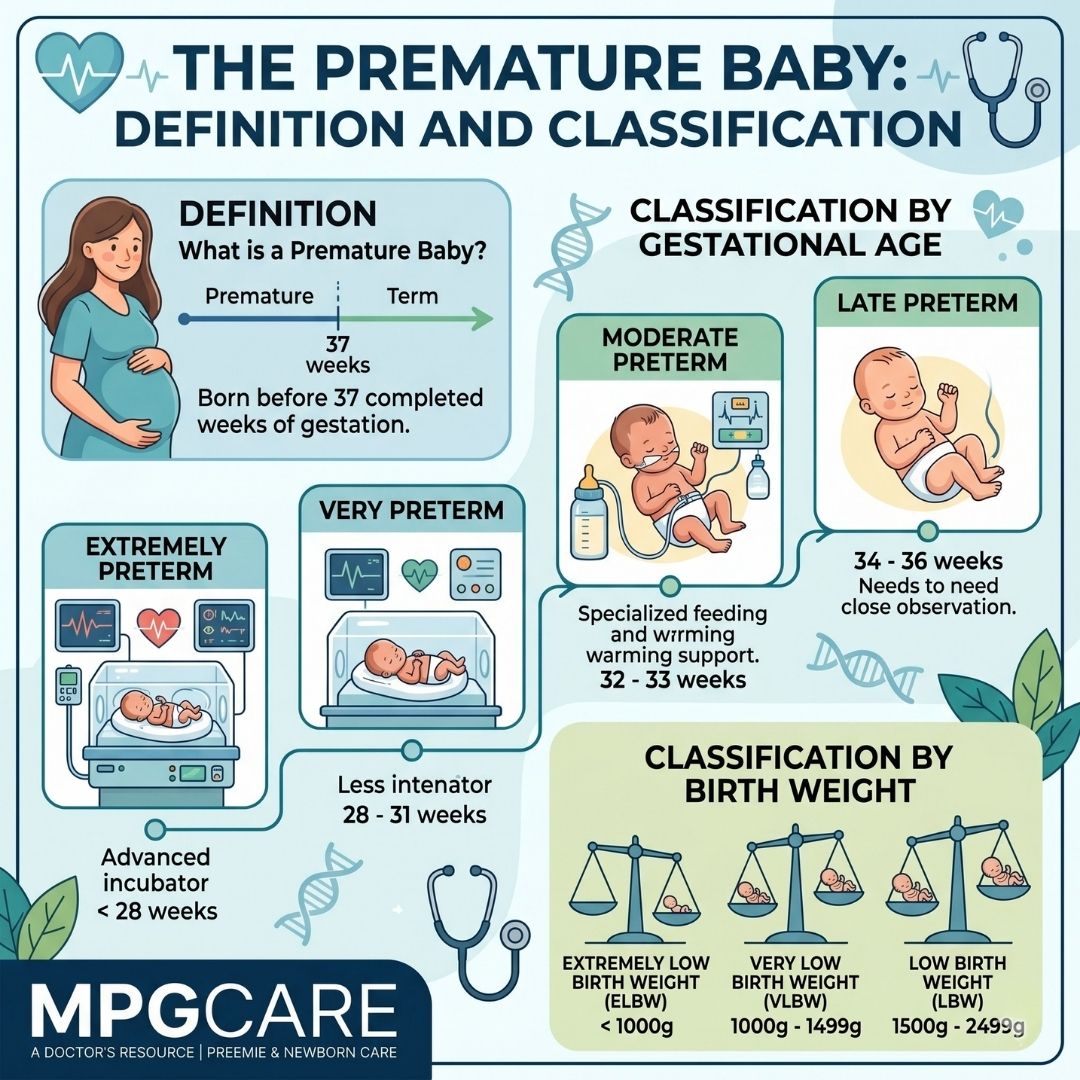
In neonatology literature, a baby is considered premature if they are born before completing 37 weeks of gestation. However, not every premature baby has the same needs.
Babies are classified according to both their birth week and birth weight. This classification is the most critical element in determining the treatment protocol to be implemented by the neonatology team.
| Classification | Birth Week |
| Late Preterm | 34 - 36 Weeks |
| Moderate Preterm | 32 - 33 Weeks |
| Very Preterm | 28 - 31 Weeks |
| Extremely Preterm | Under 28 Weeks |
The NICU (Neonatal Intensive Care Unit): What Happens Inside?
The Neonatal Intensive Care Unit (NICU) is the heart of the neonatology world. This is a living space isolated from the outside world, where temperature, humidity, and light are adjusted according to the baby's needs.
Essential Equipment in the NICU:
- Incubators: Transparent enclosures that maintain the baby's body temperature and minimize the risk of infection.
- Ventilators: Devices that provide breathing support for babies whose lungs are not yet fully developed.
- Monitors: Systems that track heart rate, respiratory rate, and blood oxygen levels every second.
- Phototherapy Units: Special blue light systems used to treat neonatal jaundice.
Neonatology nurses and specialists meticulously manage every detail, from feeding to medication, using this advanced equipment.
Most Common Problems in Premature Babies
The primary areas where neonatology focuses its efforts are the complications resulting from organ immaturity due to early birth.
Respiratory Distress Syndrome (RDS)
The lungs of premature babies often lack "surfactant," a substance that keeps the air sacs open. This leads to RDS. Neonatology specialists provide external surfactant supplements and ventilator support to allow time for the baby's lungs to develop.
Infection — Sepsis
The immune systems of babies born early are quite weak. Therefore, even a minor bacterium or virus can cause a severe infection that spreads throughout the body, known as sepsis. This is why hygiene protocols in neonatology units are of vital importance.
Hearing and Vision Issues (ROP)
In very low birth weight infants, abnormal development of blood vessels in the eye (Retinopathy of Prematurity - ROP) can occur. With regular neonatology check-ups and eye exams, permanent vision loss can be prevented. Similarly, hearing screenings are carried out without delay to detect any issues caused by medication or developmental gaps.
The Role of Parents in the NICU: Kangaroo Care
Modern neonatology approaches view the mother and father as an integral part of the treatment. At this point, one of the most effective methods is Kangaroo Care.
Skin-to-skin contact, achieved by placing the baby (wearing only a diaper) on the parent’s bare chest, works miracles.
Benefits of Kangaroo Care:
- Regulates the baby's heart rate and breathing.
- Helps maintain body temperature more effectively.
- Increases the mother’s milk production.
- Reduces stress by strengthening the bond between the baby and parent.
Discharge and Developmental Forecasting
For a baby to be discharged from a neonatology unit, they must meet specific criteria. Discharge depends more on the baby’s "life skills" than a simple "weight limit."
Discharge Criteria
- Ability to maintain body temperature at room temperature.
- Taking all feedings orally (breast or bottle).
- Consistent weight gain.
- Stable breathing and the absence of apnea (stopping breathing) spells.
Neonatology Services — MPGCare
For parents, having a premature baby can be both emotionally and financially challenging. During this sensitive period, accessing the highest quality healthcare and receiving expert support at every step is critical.
MPGCare stands by families with its deep experience and world-class technological infrastructure.
The comprehensive solutions we offer in the field of neonatology aim not only for the baby's survival but also for their healthy growth.
With our expert physician staff, high-tech NICU units, and family-oriented approach, we stand by every little warrior. At MPGCare, we continue to be the strongest supporters of miracles that arrive early, ensuring they take healthy steps toward the future.
 EN
EN













.png)









