Brain Tumor Surgery in Turkey: Advanced Technologies and Top Neurosurgeons

Brain Tumor Surgery in Turkey: Advanced Technologies and Top Neurosurgeons
Turkey has emerged as a premier global destination for neurosurgery, combining clinical excellence with some of the world’s most sophisticated medical technologies.
For patients facing a brain tumor diagnosis, the country offers a powerful synergy of highly skilled neurosurgeons and cutting-edge intraoperative tools designed to maximize tumor removal while protecting vital brain functions.
From robotic-assisted systems to advanced neuro-navigation, Turkish medical centers provide a multidisciplinary approach that prioritizes both surgical precision and patient recovery.
This guide explores the advanced technological landscape and the expertise that makes Turkey a leading choice for complex brain tumor treatments.
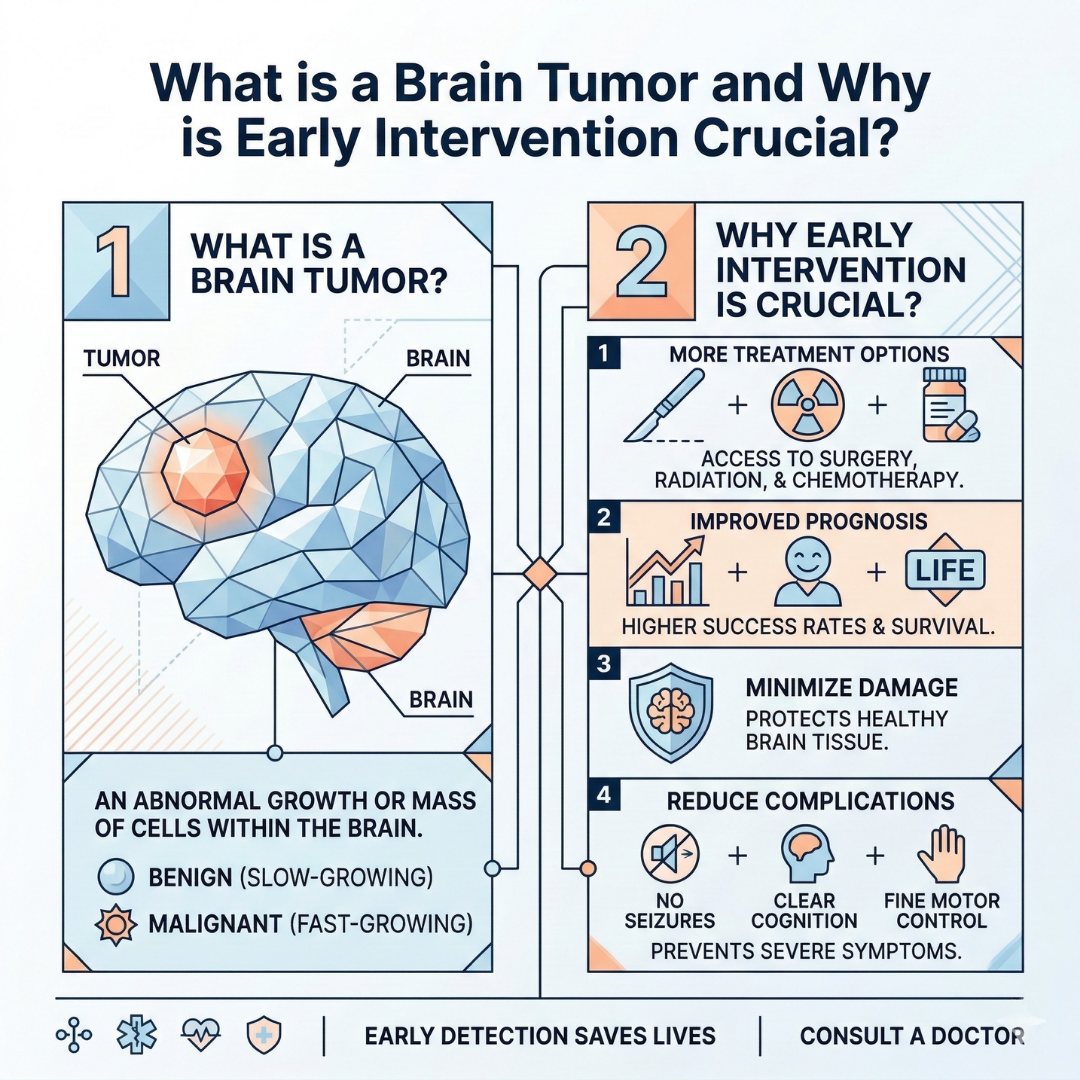
What is a Brain Tumor and Why is Early Intervention Crucial?
A brain tumor consists of abnormal cell masses that grow uncontrollably within the cranial cavity, exerting dangerous pressure on healthy brain tissue.
Regardless of whether these masses are benign (non-cancerous) or malignant (cancerous), their location alone can directly threaten vital bodily functions.
The human skull is a closed bone structure with zero capacity to expand. Therefore, any new mass growing inside increases intracranial pressure, compresses healthy cells, and leads to severe neurological deficits.
Early diagnosis and millimetric surgical precision are the most critical stages in managing brain tumors.
According to comprehensive academic research conducted in Turkey, central nervous system tumors are most frequently observed in the 50-59 age demographic.
Statistics clearly reveal that the vast majority of tumors in adult patients are located in the frontal and temporal lobes of the brain . These specific regions are the primary command centers for speech, memory, personality traits, and motor skills.
In the past, operating on these highly sensitive areas carried massive risks, such as permanent paralysis or loss of speech.
Today, the landscape has completely transformed. Advanced neurological centers in Turkey utilize state-of-the-art imaging systems to completely eradicate the tumor while flawlessly preserving healthy tissue.
A brain surgery performed at the right time, with the right technology, provenly extends survival rates and drastically improves the patient's quality of life.
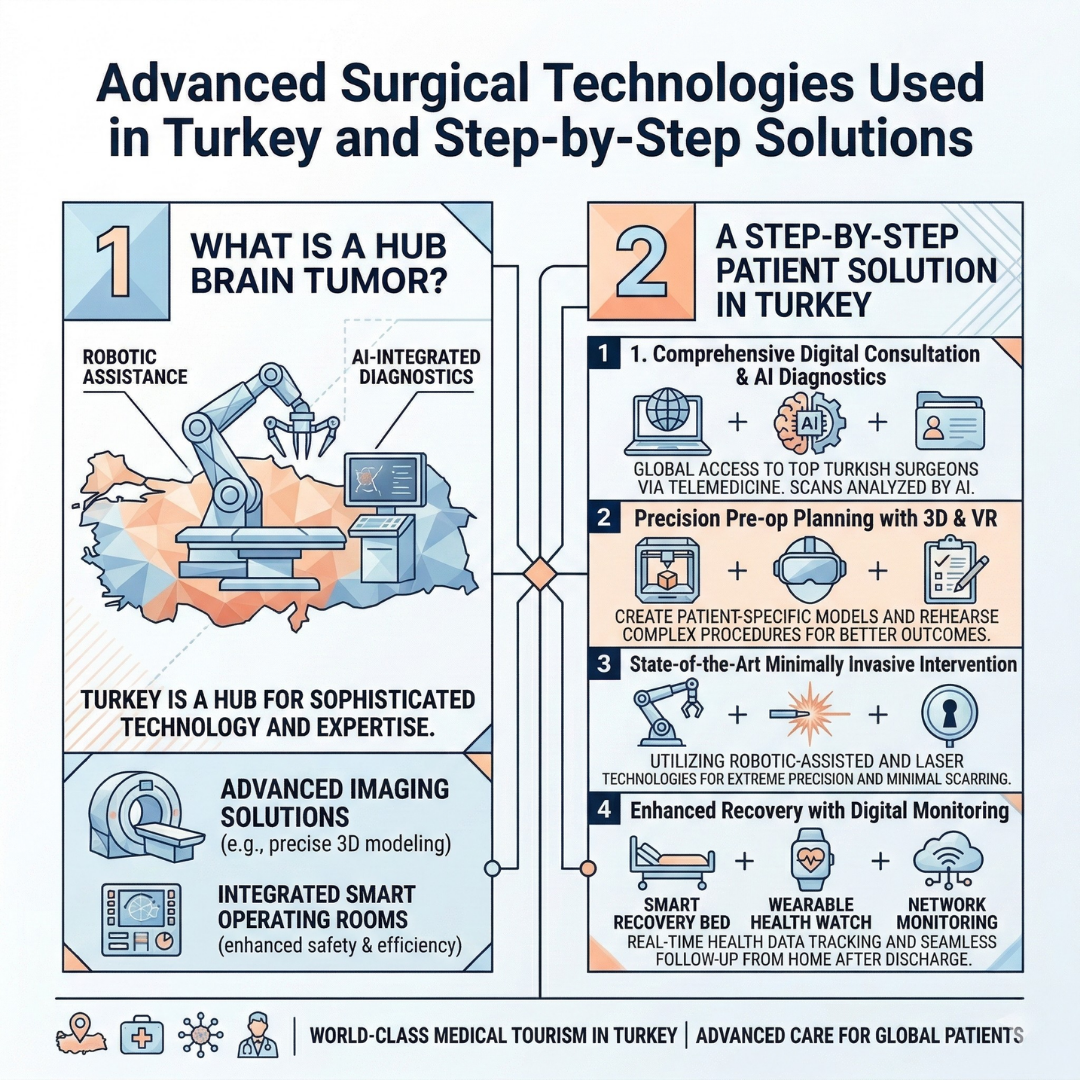
Advanced Surgical Technologies Used in Turkey and Step-by-Step Solutions
There is an unchanging golden rule in neuro-oncological tumor surgery: Extracting the maximum possible tumor tissue without causing any neurological damage (such as paralysis or sensory loss) to the patient .
To achieve this delicate balance, modern neurosurgery clinics in Turkey utilize a series of world-class technologies. Here are those life-saving systems:
1. Pre-operative Flawless Planning: Functional MRI and Tractography (DTI)
The foundation of a successful surgery is laid long before the operation begins.
Functional MRI and Tractography (DTI) technologies go far beyond standard magnetic resonance imaging by mapping the invisible 3D neural networks inside the brain .
The surgical team can visually identify the hidden neural pathways that control arm and leg movements on a computer screen.
This allows surgeons to calculate exactly how close the tumor is to vital vessels, establishing the safest surgical "corridor" into the brain.
2. Neuronavigation Systems: The Surgeon's GPS
Neuronavigation devices are the highly advanced, operating-room equivalents of the GPS systems we use in our vehicles.
The 3D brain map of the patient, created before the surgery, is loaded into this system.
During the procedure, the surgeon tracks the exact millimetric location of their surgical instruments on a monitor.
This technology makes it nearly impossible to deviate from the target, reducing the risk of healthy tissue damage to near zero.
3. Awake Craniotomy and Neuromonitoring
If a tumor is located precisely in the heart of the patient's speech or movement centers, an "Awake Craniotomy" is initiated.
The patient's scalp is numbed with local anesthesia, and during the most critical phase of tumor removal, the patient is awakened.
The surgeon converses with the patient, shows them pictures, or asks them to move their fingers while removing the mass. In a comprehensive 15-year medical study in Turkey examining 801 patients, it was proven that the rate of permanent neurological loss dropped dramatically in patients operated on via awake craniotomy .
Simultaneously, neuromonitoring devices come into play. Using tiny sensors placed in the muscles, the system instantly reads electrical signals passing through the nerves.
Even the slightest millimetric approach to the wrong tissue triggers an instant alarm, commanding the surgeon to stop.
4. Intraoperative Imaging (Intraoperative MRI and Ultrasound)
These systems eliminate the dangerous doubt of "Has the tumor been completely removed?" during the operation.
While the surgery is still ongoing and the skull is open, an ultrasound or MRI scan is performed directly in the surgical field. If even a grain-sized tumor cell remains, it is instantly detected, and the procedure is completed right there.
|
Comparison Criteria |
Traditional Surgical Methods |
Advanced Tech-Assisted Surgery (2026) |
|
Location Tracking |
Relies entirely on the surgeon's theoretical anatomical knowledge |
Millimetric 3D positioning via Neuronavigation |
|
Margin Control |
Relies on visual estimation and surgical experience |
Instant verifiable proof via Intraoperative MRI/Ultrasound |
|
Function Preservation |
Results are unknown until the patient wakes up post-op |
Real-time speech and movement testing via Awake Craniotomy |
|
Nerve Damage Risk |
Carries a high risk of neurological damage (paralysis) |
Minimum risk achieved through continuous Neuromonitoring |
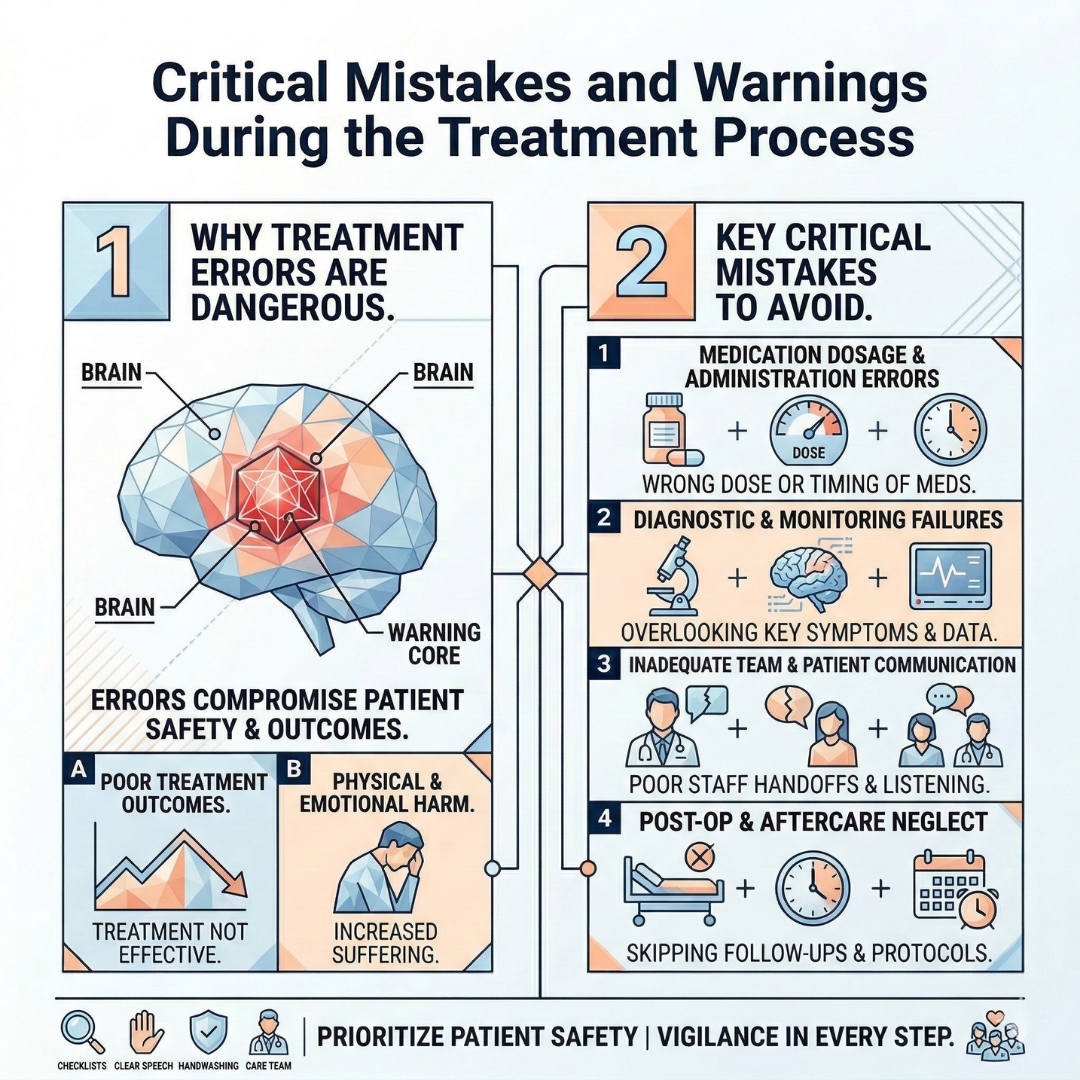
Critical Mistakes and Warnings During the Treatment Process
When dealing with a brain tumor suspicion or a definitive diagnosis, patients frequently fall into common traps that can severely disrupt the treatment process.
The first and biggest mistake is ignoring the signals the body sends. Persistent morning headaches, unexplained nausea, sudden blurred vision, or abrupt personality changes are often mistakenly attributed to "stress" or "fatigue." However, every month lost before medical intervention means increased pressure inside the brain and further tumor expansion .
Early diagnosis ensures the mass is removed while it is small, preventing permanent damage.
The second fatal error is pursuing unscientific alternative methods. Extreme fear of brain surgery can push patients toward hearsay information, herbal remedies, or unproven alternative treatments.
The scientific reality is that no herbal mixture can eradicate a growing mass from brain tissue. The time wasted on these methods often allows the tumor to grow beyond operable limits.
Finally, choosing an inadequately equipped medical center is one of the biggest barriers to recovery. Brain tumor surgery is not solely about individual surgical skill; it is highly dependent on an advanced medical team and technological infrastructure.
Undergoing this procedure in a facility lacking neuronavigation, intraoperative MRI, neuromonitoring, or comprehensive intensive care units turns the chances of success into a dangerous gamble.
Frequently Asked Questions
How long does a brain tumor surgery take?
The duration of the surgery varies based on the size of the tumor, the specific lobe of the brain it is located in, and the technology applied. However, comprehensive neuro-oncological surgeries supported by advanced devices generally take between 4 to 8 hours to complete.
Does brain tumor surgery carry a fatal risk?
Compared to previous decades, modern technologies (such as neuromonitoring, neuronavigation, and microscopic surgery) have radically reduced complication rates. When performed in fully equipped centers by experienced multidisciplinary teams, the surgical risks are kept to an absolute minimum .
Do patients feel pain during an awake brain surgery?
No, patients do not feel pain. The brain tissue itself lacks the receptors required to perceive pain. The skull and skin incision areas are completely numbed with local anesthesia at the beginning of the surgery. Although patients are awake during the procedure, they only feel light touches, never sharp pain.
What is the recovery process like after surgery?
Following surgeries performed with advanced techniques, patients are typically kept under observation in the intensive care unit for 1 or 2 days, then transferred to a standard room. In the absence of complications, patients are generally discharged within 5 to 7 days. Most individuals can return to their basic daily routines within two weeks.
Conclusion and Next Steps
Although receiving a brain tumor diagnosis may initially seem like the beginning of a dark and uncertain path, the point medical science has reached today is incredibly promising.
Thanks to the awake craniotomies, 3D neuronavigation, and functional mapping techniques routinely applied in Turkey, brain surgeries are no longer a step into the unknown; they are highly predictable and safe procedures.
Instead of ignoring the illness or surrendering to unnecessary fears, utilizing these technological advancements is the smartest step a patient can take.
When it comes to neurological health, time is either the greatest ally or the worst enemy. If persistent neurological symptoms are present, or a tumor diagnosis has recently been made, do not waste time.
Take action today by consulting a fully equipped neurological center with an advanced technological infrastructure and a multidisciplinary expert team. Do not delay the treatment; regain control of the future starting right now.
 EN
EN






.png)









